http://rarediseases.info.nih.gov/gard/7300/pachygyria/case/24499/case-questions
This information was updated on 2/20/14
What is pachygyria?
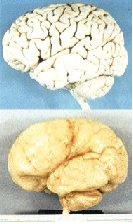
Pachygyria is a developmental condition due to abnormal migration of nerve cells (neurons) in the developing brain and nervous system.[1] With pachygyria, there are few gyri (the ridges between the wrinkles in the brain), and they are usually broad and flat. The condition is also known as “incomplete lissencephaly.”[2][3] Pachygyria may occur alone (isolated) or as part of various underlying syndromes. Symptoms vary among affected people and may include moderate to severe developmental delay, seizures, poor muscle tone and control, feeding or swallowing difficulties, and small head size (microcephaly).[1][3] In most cases it is not inherited, but various inheritance patterns have been reported.[1][4] Treatment is symptomatic and supportive.[1][2]
What are the signs and symptoms of pachygyria?
Signs and symptoms of pachygyria vary among affected people and can depend on the extent of the abnormality. They often include poor muscle tone and motor function; seizures; developmental delays; intellectual disability; failure to grow and thrive; difficulties with feeding or swallowing; swelling in the extremities; and small head size (microcephaly). Most infants appear physically normal, but some conditions associated with pachygyria cause distinctive facial or skull characteristics.[1]
What causes pachygyria?
Pachygyria, also called “incomplete lissencephaly,” may be caused by various non-genetic (environmental) and genetic factors that play a role in impairing the development of the outer region of the brain (the cerebral cortex).[5] The cerebral cortex is responsible for conscious movement and thought, and should have deep convolutions (gyri) and grooves (sulci), which are formed by “infolding” of the cerebral cortex. During normal embryonic growth, immature cells that later develop into specialized nerve cells (neurons) normally migrate to the brain’s surface, making several layers of cells. When this process is impaired, the cells don’t migrate to their locations, resulting in too few cell layers and absence (agyria) or incomplete development (pachygyria) of gyri.[5]
Environmental factors that contribute to the condition may include intrauterine infection during pregnancy (such as a virus), and insufficient flow of oxygenated blood to the brain (ischemia) during fetal development.[5]
More than 25 syndromes due to abnormal migration of neurons have been reported; in some of these cases, the genetic cause and pattern of inheritance depends on that of the specific syndrome.[1][4]
Mutations in several genes have been identified in people with abnormalities of cortical development, including the KIF5C, KIF2A, DYNC1H1, WDR62, and TUBG1 genes.[6] Studies have also found that isolated lissencephaly may result from mutations in the LIS1 and XLIS (also called DCX) genes.[5]
People interested in learning about the cause of pachygyria in themselves or family members should speak with their health care provider or a a genetics professional.
How might pachygyria be treated?
Because the symptoms of the condition vary from person to person, treatment is symptomatic, and may include anti-seizure medication, such as Trileptal, and special or supplemental education consisting of physical, occupational, and speech therapies.[1][2]
What is the long-term outlook for people with pachygyria?
The long-term outlook (prognosis) varies depending on the underlying cause, the degree of brain abnormality and subsequent neurological losses.[1]
References
NINDS Neuronal Migration Disorders Information Page. National Institute of Neurological Disorders and Stroke (NINDS) Web site. 2007; http://www.ninds.nih.gov/health_and_medical/disorders/neuronal_migration.htm. Accessed 8/18/2009.
Grainger & Allison’s Diagnostic Radiology: A Textbook of Medical Imaging, 4th ed.. 2001;
Pachygyria. The Cortical Foundation. 2012; http://cortfoundation.org/cms/pachygyria/. Accessed 2/20/2014.
Straussberg R, Gross S, Amir J, Gadoth N. A new autosomal recessive syndrome of pachygyria. Clin Genet. 1996; http://www.ncbi.nlm.nih.gov/pubmed/9147882. Accessed 8/18/2009.
LISSENCEPHALY. NORD. September 6, 2012; https://www.rarediseases.org/rare-disease-information/rare-diseases/byID/454/viewAbstract. Accessed 2/20/2014.
Poirier K et. al. Mutations in TUBG1, DYNC1H1, KIF5C and KIF2A cause malformations of cortical development and microcephaly. Nat Genet. June, 2013; 45(6):639-647. Accessed 2/20/2014.


